The Best Probiotics for Gum Disease Prevention and Teeth Whitening
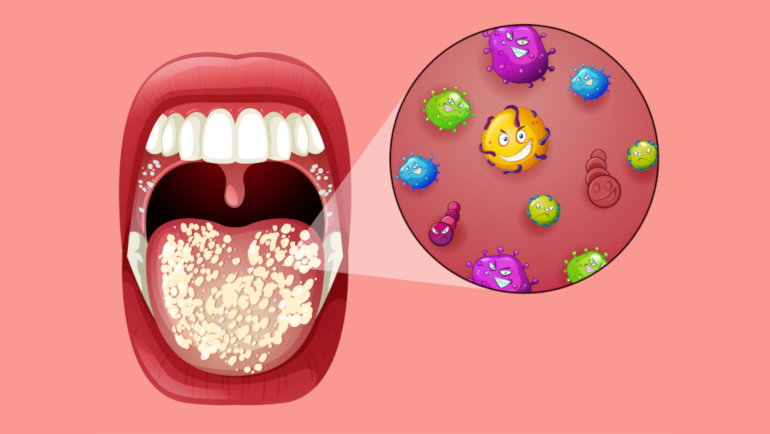
The oral microbiome, a complex ecosystem of bacteria residing in the mouth, plays a crucial role in maintaining oral health. An imbalance in this ecosystem, known as dysbiosis, can lead to various oral diseases, including gingivitis, periodontitis (gum disease), and even contribute to systemic health issues. Conversely, a balanced and healthy oral microbiome, fostered by beneficial bacteria, can contribute to improved gum health and potentially even enhance teeth whitening. This article explores the potential of probiotics in promoting oral health, specifically focusing on their role in gum disease prevention and teeth whitening.
Understanding the Oral Microbiome and its Impact on Oral Health
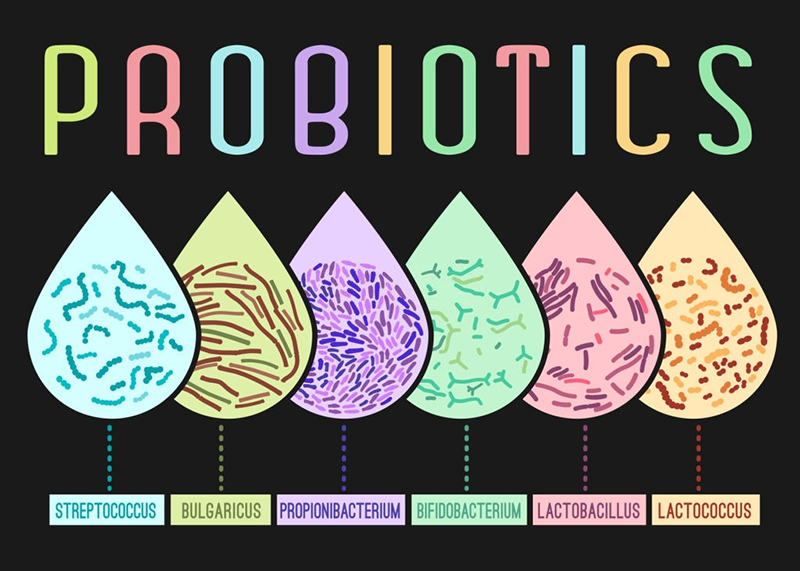
The human mouth harbors hundreds of bacterial species, some beneficial and some harmful. A healthy oral microbiome is characterized by a delicate equilibrium between these populations. Beneficial bacteria, such as certain strains of Streptococcus and Lactobacillus, contribute to maintaining oral hygiene by producing antimicrobial substances and competing with pathogenic bacteria for resources. However, factors like poor oral hygiene, smoking, genetics, and underlying health conditions can disrupt this balance, leading to a dominance of harmful bacteria.
The Role of Dysbiosis in Gum Disease
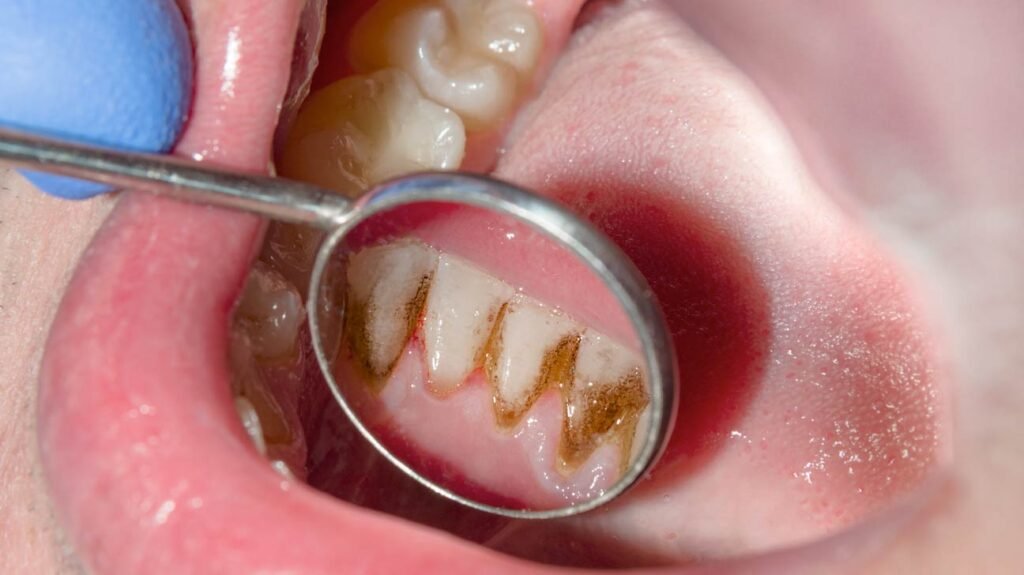
Dysbiosis, or an imbalance in the oral microbiome, is a hallmark of gum disease. Pathogenic bacteria, such as Porphyromonas gingivalis, Tannerella forsythia, and Aggregatibacter actinomycetemcomitans, proliferate, producing inflammatory molecules that damage the gums and supporting structures of the teeth. This inflammation leads to gingivitis, characterized by red, swollen, and bleeding gums. If left untreated, gingivitis can progress to periodontitis, a more severe form of gum disease that can result in tooth loss.
The Link Between Oral Health and Systemic Health
Emerging research highlights the strong connection between oral health and systemic health. Bacteria associated with gum disease can enter the bloodstream and contribute to conditions like cardiovascular disease, diabetes, and respiratory infections. Maintaining a healthy oral microbiome is therefore crucial not only for oral health but also for overall well-being.
Probiotics: A Potential Therapeutic Approach
Probiotics, defined as live microorganisms that confer a health benefit on the host when administered in adequate amounts, are increasingly recognized for their potential in preventing and treating various diseases. In the context of oral health, probiotics offer a promising avenue for restoring the balance of the oral microbiome and improving gum health.
Mechanisms of Action of Probiotics in Oral Health
Probiotics exert their beneficial effects through various mechanisms, including:
- Competition for resources and adhesion sites: Probiotics compete with pathogenic bacteria for nutrients and attachment sites on the teeth and gums, limiting their colonization and growth.
- Production of antimicrobial substances: Certain probiotics produce bacteriocin-like inhibitory substances, hydrogen peroxide, and organic acids that inhibit the growth of pathogenic bacteria.
- Modulation of the immune system: Probiotics can modulate the host's immune response, reducing inflammation and promoting tissue repair.
- Enhancement of the epithelial barrier: Probiotics can strengthen the integrity of the gum tissue, reducing its permeability to harmful bacteria and their products.
Specific Probiotic Strains with Potential Benefits
While research is ongoing, several probiotic strains have shown promise in improving oral health:
- Lactobacillus reuteri: Studies suggest that this strain can reduce gingivitis and plaque formation.
- Lactobacillus salivarius: This strain exhibits antimicrobial activity against several pathogenic bacteria associated with gum disease.
- Streptococcus salivarius K12: This strain has demonstrated potential in preventing dental caries and reducing gingivitis.
- Weissella cibaria: This strain has shown promise in reducing periodontal inflammation.
It is important to note that the efficacy of probiotics can vary depending on the strain, dosage, delivery method, and individual characteristics. Further research is needed to establish definitive guidelines for the use of probiotics in oral health.
Probiotics and Teeth Whitening
While the primary focus of probiotic research in oral health is on gum disease prevention, some evidence suggests a potential link between probiotics and teeth whitening. This is largely indirect, as probiotics contribute to a healthier oral environment that may reduce staining factors.
Indirect Effects on Teeth Whitening
A healthy oral microbiome, supported by probiotics, can contribute to teeth whitening indirectly through several mechanisms:
- Reduced plaque formation: Probiotics can reduce the accumulation of plaque, a major contributor to tooth staining.
- Improved gum health: Healthy gums are less prone to bleeding, which can exacerbate staining.
- Reduced inflammation: Inflammation can contribute to changes in tooth color. Probiotics, by reducing inflammation, may indirectly improve tooth appearance.
It is crucial to understand that probiotics are not a replacement for professional teeth whitening treatments. They may contribute to a healthier oral environment that supports naturally whiter teeth, but they are not a direct whitening agent.
Choosing and Using Probiotic Products for Oral Health
Selecting appropriate probiotic products for oral health requires careful consideration. Look for products that:
- Specify the strain(s) of probiotics included.
- Indicate the number of colony-forming units (CFUs) per dose.
- Are formulated specifically for oral use (e.g., lozenges, mouthwashes).
- Are manufactured under good manufacturing practices (GMP).
Consult with a dentist or other healthcare professional before incorporating probiotics into your oral hygiene routine, especially if you have pre-existing medical conditions. They can provide personalized recommendations and address any concerns.
Conclusion
The potential of probiotics in improving oral health is significant. While research is still ongoing, evidence suggests that specific probiotic strains can effectively contribute to the prevention of gum disease by restoring the balance of the oral microbiome. Although not a direct teeth whitening agent, a healthy oral environment fostered by probiotics can indirectly support naturally whiter teeth. However, maintaining good oral hygiene practices, such as regular brushing, flossing, and professional dental cleanings, remain essential for optimal oral health. The integration of probiotics should be considered as a complementary strategy, not a replacement, for established oral hygiene protocols. Always consult with a dental professional for personalized advice and to address any specific concerns regarding your oral health.