Unlocking the Power of Neem: Your Guide to Natural Oral Care
Hey there! So you're curious about neem and its potential benefits for your oral health? You've come to the right place! Neem, derived from the neem tree (Azadirachta indica), has been used for centuries in Ayurvedic medicine, and its amazing properties are finally getting the recognition they deserve in the Western world. Let's dive into how you can harness the power of neem for a healthier, happier mouth.What Makes Neem So Special for Oral Health?
Neem's magic lies in its active compounds, particularly nimbin, azadirachtin, and nimbidin. These aren't just fancy names; they're potent natural fighters against the bacteria, fungi, and viruses that contribute to common oral problems. Think plaque, gingivitis, bad breath â€" neem can tackle them all!
Here's the breakdown of its superstar qualities:
- Antibacterial Powerhouse: Neem's strong antibacterial properties effectively combat the bacteria responsible for plaque buildup and gum inflammation. It's like a tiny army fighting off the invaders in your mouth!
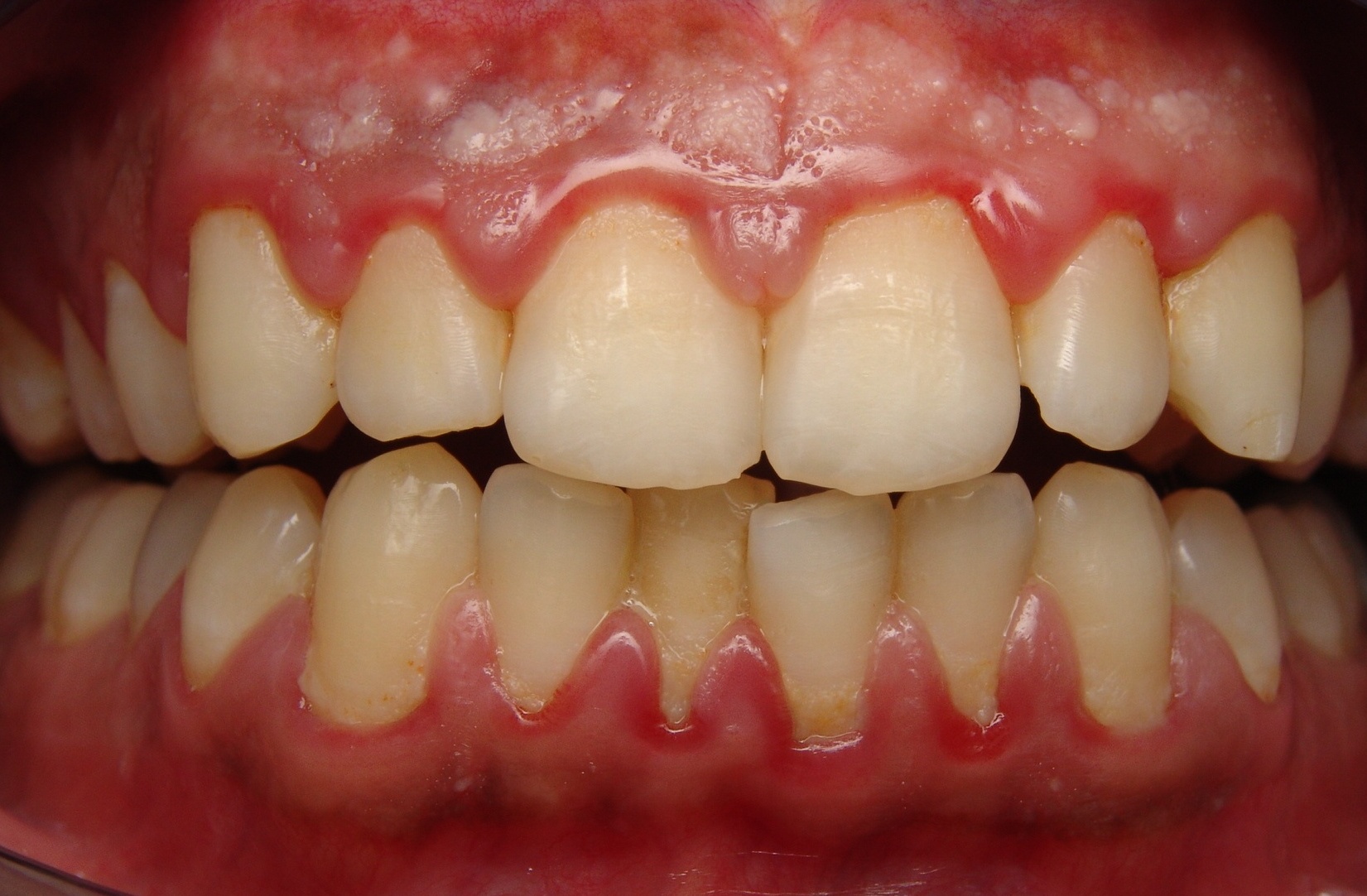
- Anti-inflammatory Effects: Inflammation is at the root of many gum diseases. Neem's anti-inflammatory action helps soothe irritated gums and reduce swelling.
- Anti-fungal Properties: Oral thrush, a fungal infection, can be uncomfortable and persistent. Neem's antifungal properties can help keep those pesky fungi in check.
- Antiviral Action: While less researched than its other properties, neem also shows potential antiviral effects, which could be beneficial in fighting off certain oral viruses.
- Wound Healing: Neem can help promote healing in minor oral wounds, such as small cuts or sores, speeding up recovery time.
How to Incorporate Neem into Your Oral Care Routine
There are several ways to bring the benefits of neem into your daily oral hygiene:
Neem Toothpaste
This is probably the easiest way to start! Look for toothpastes that specifically list neem extract as a key ingredient. Many natural brands offer neem toothpastes that combine its benefits with other natural ingredients like fluoride (for cavity prevention) or essential oils for extra freshness.
Tip: Start slowly. Some people find that neem toothpaste has a slightly bitter taste at first. If it's too strong, you can try mixing it with your regular toothpaste until you get used to the flavor.
Neem Oil Pulling
Oil pulling, an ancient Ayurvedic practice, involves swishing oil around in your mouth to draw out bacteria and toxins. Neem oil is particularly effective for this because of its potent antibacterial properties.
How to do it: Take about a tablespoon of neem oil (make sure it's specifically designed for oral use) and swish it gently around your mouth for 15-20 minutes. Spit it out into the trash (never the sink, as it can clog your pipes), and rinse your mouth thoroughly with water. Do this once a day, preferably in the morning before brushing your teeth.
Important Note: Neem oil can be quite potent, so start with shorter sessions (5-10 minutes) and gradually increase the time. Some people experience mild tingling or a slightly bitter taste; this is normal, but if you experience discomfort, reduce the duration or frequency of oil pulling.
Neem Mouthwash
You can either buy commercially available neem mouthwashes or make your own by diluting neem oil in water (a few drops in a glass of water). Swish this mixture around your mouth for 30 seconds to a minute, then spit it out and rinse with plain water. This is a great way to freshen breath and give your mouth an extra dose of neem's antibacterial power.
Caution: Don't swallow neem oil or mouthwash. It's for external use only.
Neem Sticks (Datun)
Traditional neem sticks, or datun, are twigs from the neem tree that are chewed on like a toothbrush. They have been used for centuries in many cultures for oral hygiene. The fibers act like bristles, while the neem extracts provide the antibacterial benefits. If you can find authentic neem sticks, they're a truly unique and natural approach to brushing your teeth.
Note: The texture might take some getting used to. It's not as soft as a regular toothbrush, and you may need to chew on the stick to create soft bristles.
Beyond Brushing: The Holistic Neem Approach
Incorporating neem into your oral care routine is just one aspect of maintaining good overall oral health. Remember to:
- Brush and floss regularly: Neem is a powerful supplement, but it shouldn't replace good brushing and flossing habits.
- Maintain a healthy diet: A balanced diet low in sugar and refined carbohydrates helps prevent cavities and gum disease.
- Drink plenty of water: Staying hydrated is crucial for overall health, including the health of your mouth.
- Visit your dentist regularly: Regular checkups and cleanings are essential for detecting and treating any oral health problems early on.
Possible Side Effects and Precautions
While generally safe, neem can cause some side effects in a few individuals. These can include:
- Mild tingling or burning sensation in the mouth
- Slight bitterness
- Allergic reactions (rare)
If you experience any severe reactions, stop using neem products immediately and consult a doctor or dentist.
Important: Pregnant or breastfeeding women should consult their doctor before using neem products, as research on its safety during pregnancy and breastfeeding is limited.
Frequently Asked Questions
Q: Is neem oil safe to swallow?
A: No, neem oil is not intended for ingestion. It's for external use only in oral care.
Q: How long does it take to see results from using neem for oral health?
A: Results vary from person to person. Some people report noticing improvements in their gum health and breath within a few weeks of consistent use. Others may see more significant changes over a longer period.
Q: Can I use neem products if I have sensitive teeth?
A: Some people with sensitive teeth may find that neem products cause a slight tingling or burning sensation. Start with a small amount and gradually increase usage to see how your teeth react. If you experience significant sensitivity, reduce usage or discontinue use.
Q: Where can I buy neem products?
A: Neem products are widely available online and in many health food stores and pharmacies.
Q: Can neem cure gum disease?
A: Neem can help manage and improve symptoms associated with gum disease, but it's not a cure. For severe gum disease, professional dental treatment is essential.
I hope this comprehensive guide helps you incorporate neem into your oral care routine! Remember, consistency is key. With regular use, you can unlock the many benefits of this amazing natural remedy. Happy brushing (or swishing or chewing â€" whichever method you choose!)









).jpg)